- Aretha Franklin, the 76-year-old “Queen of Soul,” has died of advanced neuroendocrine pancreatic cancer
- Her death brings to light just how deadly pancreatic cancer is-as early detection is extremely difficult for doctors
- Understanding your risk factors and learning to spot the symptoms that do appear are crucial to survival
Aretha Franklin-known as the “Queen of Soul” and for her hit song “Respect”-has died of pancreatic cancer at 76 years old, The Associated Press reports.
Her publicist confirmed through a family statement: “Franklin’s official cause of death was due to advanced pancreatic cancer of the neuroendocrine type, which was confirmed by Franklin’s oncologist, Dr Philip Phillips.”
Franklin’s death highlights one of the most insidious cancers out there. While pancreatic cancer only accounts for about 2.5 percent of all cancer cases, it makes up 6 percent of cancer deaths, according to Cancer Australia. So while it’s relatively rare, it’s extremely deadly-and has seen an uptick in recent years.
But why does pancreatic cancer in particular seem to stump doctors? Here’s why it can be so difficult to detect the disease early on and what you should know about your risk.
What is pancreatic cancer-and why is it so deadly?
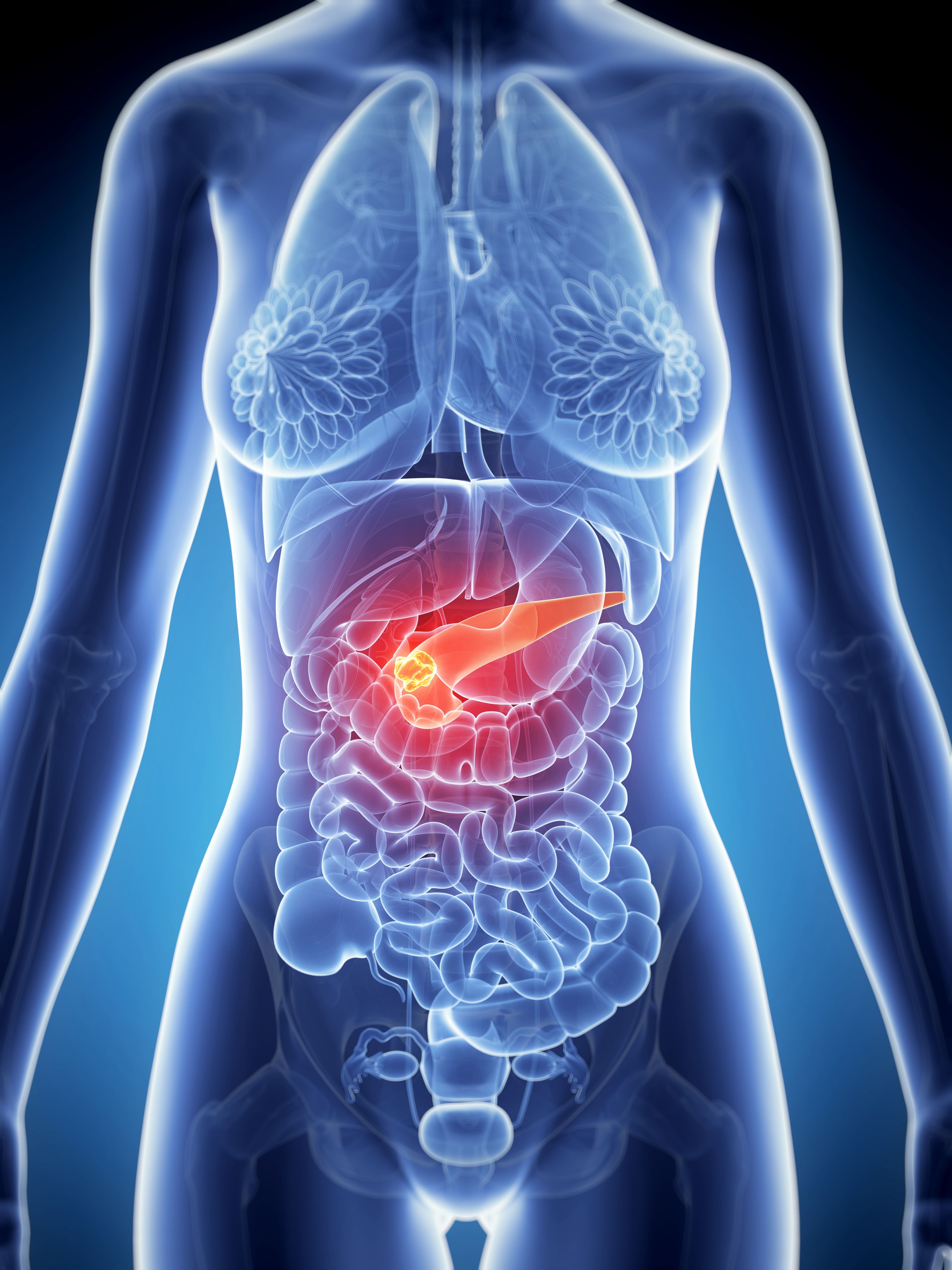
First, some background on your pancreas: the organ is about 6 inches long and located behind your stomach, where it produces digestive juices to help your body break down food, and insulin to help regulate your blood sugar levels.
When cells in your pancreas start to multiply and grow out of control at a rapid pace, cancerous tumours can develop. There are two types of cells-exocrine and endocrine-that can form these tumors. Exocrine pancreatic cancer is by far the most common, says the ACS. Neuroendocrine tumours (the type that Franklin was diagnosed with) actually makes up less than 5 percent of all pancreatic cancers.
The problem: it’s extremely hard to detect these tumours, regardless of the type. There are currently no early-detection tests available, so doctors have no way of performing screening like they do for, say, breast or colon cancers. And when it comes to neuroendocrine tumours, benign (noncancerous) cells are difficult to differentiate from malignant (cancerous) ones, making the process even trickier, the ACS states.
Pancreatic cancer is nearly invisible until it’s already advanced to a more aggressive stage.
Your anatomy kind of gets in the way, too. Your gastrointestinal tract consists of several different organs, all of which form complex layers within your body. Some layers are thick, while others are much thinner, according to gastrointestinal cancer specialist Dr William Grady.
For example, colon cancer is easier to catch at an early stage because it’s surrounded by a thicker layer of tissue and organs-meaning the cancer can’t spread to other areas of your body as quickly, giving your doctor time to detect it (there are screening tests!) and offer treatment before it goes on to an advanced, more dangerous stage.
But the area surrounding your pancreas is really quite thin, so the cancer has an easier time moving beyond your pancreas to other parts of your body, where it picks up momentum and becomes more aggressive. What’s more, your pancreas resides deeper within your body, so even if a tumour was present, your doctor would have a hard time feeling it during a normal checkup.
That’s the thing: pancreatic cancer is nearly invisible-that is, until it’s already progressed to a more advanced, harder-to-treat stage.
What are the symptoms of pancreatic cancer?
The most common warning signs of pancreatic cancer include abdominal or back pain, unexplained blood clots, lack of appetite or unusual weight loss, nausea, and diarrhoea or floating stools. Seems pretty random, right?
That’s a huge issue: the symptoms of pancreatic cancer are so nonspecific that they can be written off as a different health problem, which delays earlier diagnosis, says Dr Grady.
The most unique symptoms to keep your eyes peeled for is jaundice (yellowing of your skin and eyes), but by the time this happens, the cancer has likely already spread to your liver.
So is there anything you can do to prevent pancreatic cancer?
While there are no screening tests available now, doctors are working on figuring out a way to spot pancreatic cancer in its earlier stages. Research suggests that precancerous lesions may form on your pancreas (similar to the way they precancerous polyps form on your colon), so that has been a starting point, says Dr Grady.
Until then, know that there are certain factors that significantly raise your risk of pancreatic cancer. (Keep in mind that these are better understood for the more common exocrine tumours, rather than the rare neuroendocrine ones that led to Franklin’s death.)
Up to 30 percent of cases may be caused by smoking cigarettes-so if lung cancer wasn’t enough of a concern, tack this one onto the list. Maintaining a healthy weight is also crucial, as those who are obese (defined as a BMI of 30 or higher) are 20 percent more likely to deal with pancreatic cancer. Even carrying extra weight without developing full on obesity can be risky.
Then, there are certain factors you can’t do much about. First, inheriting certain gene mutations-like BRCA1, BRCA2, PRSS1 genes, and others-can be a problem. These mutations may trigger 10 percent of pancreatic cancer cases. (You can be tested for BRCA mutations and discuss options with your doctor if you get a positive result, as it is strongly linked to breast and ovarian cancers, too.)
A majority of people who are diagnosed with pancreatic cancer are 65 or older (Franklin was 76 years old at the time of her death).
So what does this mean for you? Eating a healthy diet, exercising regularly, and kicking your smoking habit can help you prevent not only pancreatic cancer, but also a number of other serious diseases. If you are in a higher risk group, don’t write off “everyday” symptoms, thinking they’ll just go away. See your doc if you feel like something is wrong-it may be more serious than you think.






.png&h=193&w=250&c=1&s=1)

.png&h=193&w=250&c=1&s=1)
